FAQs about PNH symptoms
People with paroxysmal nocturnal hemoglobinuria (PNH) commonly experience attacks when symptoms suddenly worsen, which can be brought on by stressors like infection and trauma. Outside of these attacks, symptoms tend to ease. Modern therapies can help to ease PNH symptoms. In very rare cases, the symptoms of the disease resolve on their own, a phenomenon known as spontaneous remission.
Symptoms of paroxysmal nocturnal hemoglobinuria (PNH) may get worse over time, as ongoing blood cell damage puts continual stress on bodily systems. However, there is a lot of variation in how PNH symptoms change over time, and some patients may have stable disease for years, especially with modern therapy. People with PNH also may experience attacks when symptoms suddenly worsen, which can occur in response to triggers like physical exertion, infections, or stress.
There is wide variation in the rate of progression for symptoms of paroxysmal nocturnal hemoglobinuria (PNH). Some people with the disease may have relatively mild symptoms that are stable for many years, whereas in others the disease can rapidly progress to cause life-threatening symptoms.
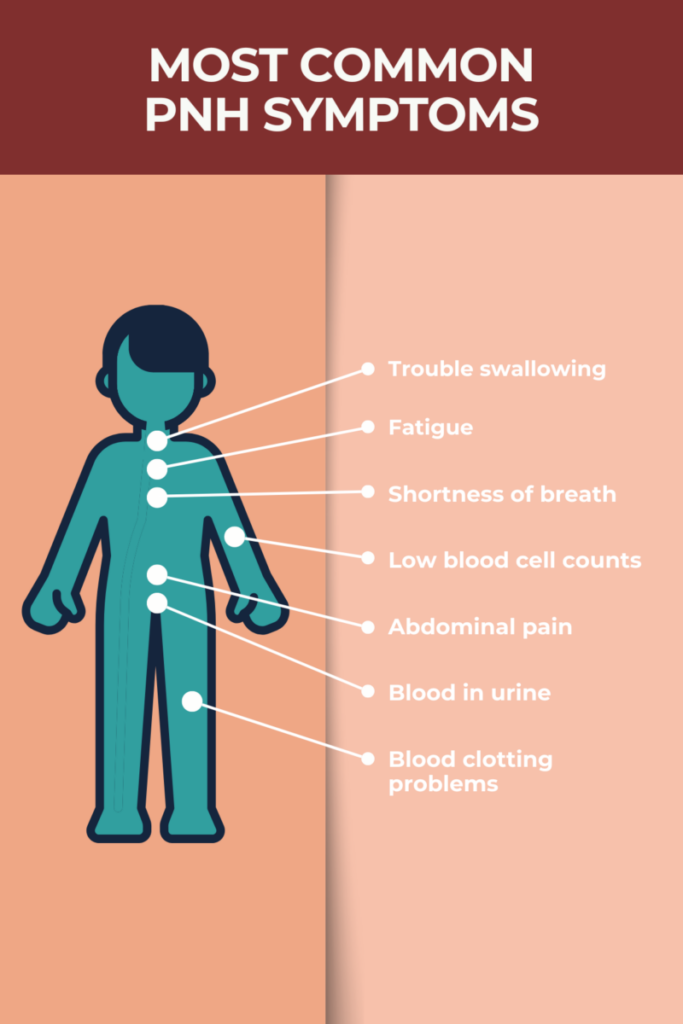
Paroxysmal nocturnal hemoglobinuria (PNH) is characterized by blood cells breaking apart. Common symptoms include reddish or brown urine, low blood cell counts, fatigue and weakness, shortness of breath, difficulty swallowing, abdominal pain, and blood clotting problems.
Paroxysmal nocturnal hemoglobinuria (PNH) can develop anytime between early childhood and later in life, but symptoms of the disease most commonly appear between ages of 30 and 40.
 Fact-checked by
Fact-checked by